It’s interesting how patterns appear in clinic.
This week alone, I treated several patients for excessive sweating, mainly underarms and hands, and it reminded me how impactful this condition can be when people finally seek treatment.
With summer approaching, it becomes more noticeable. But for most patients, this is not a seasonal issue. It is something they have often lived with for years.
What is hyperhidrosis?
Hyperhidrosis is excessive sweating that goes beyond what the body needs to regulate temperature.
It is typically caused by overactivity of the sympathetic nervous system, which overstimulates sweat glands, even when the body doesn’t need cooling.
This is why some patients notice sweating even when they are not hot, or even when they feel cold. It can feel disproportionate to the situation, and often confusing.
There are two main types:
- Primary hyperhidrosis: usually starts in childhood or adolescence and affects specific areas (underarms, hands, feet, scalp)
- Secondary hyperhidrosis: caused by an underlying factor such as medications, hormonal changes, or medical conditions
The most commonly treated area is the underarms, where it can be particularly visible and difficult to manage.
Hands are another big one, and often the most functionally frustrating. Patients describe:
- Difficulty shaking hands
- Struggling to hold a phone
- Damp keyboards when typing
It is not dangerous. But it can have a real impact on confidence and day-to-day life.
The day-to-day reality
What patients often describe is not just sweating, but the constant awareness of it.
- Glasses slipping down the nose
- Hair looking greasy despite being freshly washed
- Needing to plan clothing carefully
- Feeling self-conscious in meetings or social settings
It becomes something that sits in the background of everything.
How can excessive sweating be treated?
There are several options, depending on the area and severity.
Topical treatments
Stronger clinical antiperspirants (such as aluminium chloride-based products) can help in mild cases, although irritation is common.
Iontophoresis
Used mainly for hands and feet. Some patients see good results, but it requires regular ongoing sessions to maintain improvement.
Energy-based treatments
MiraDry reduces sweat glands in the underarm using thermal energy.
A simple way to think about the difference:
- Botox turns the tap off completely, but temporarily
- MiraDry turns the tap down, more permanently
Radiofrequency microneedling (RFM) is also being used in some settings to target sweat glands and reduce activity, with emerging evidence supporting its use.
Botox
Botox remains the most reliable and predictable treatment we use in clinic. It works by blocking the nerve signals that stimulate the sweat glands. Without that signal, the glands do not produce sweat in the treated area.
Patients often ask how long it lasts. In most cases, results are seen within 1–2 weeks and last around 4 to 6 months.
Treatment can then be repeated as needed.
Underarm treatment in particular is generally very well tolerated.
Surgical options
In more severe, treatment-resistant cases, procedures such as endoscopic thoracic sympathectomy can be considered, although this is rarely required.
What is the treatment like?
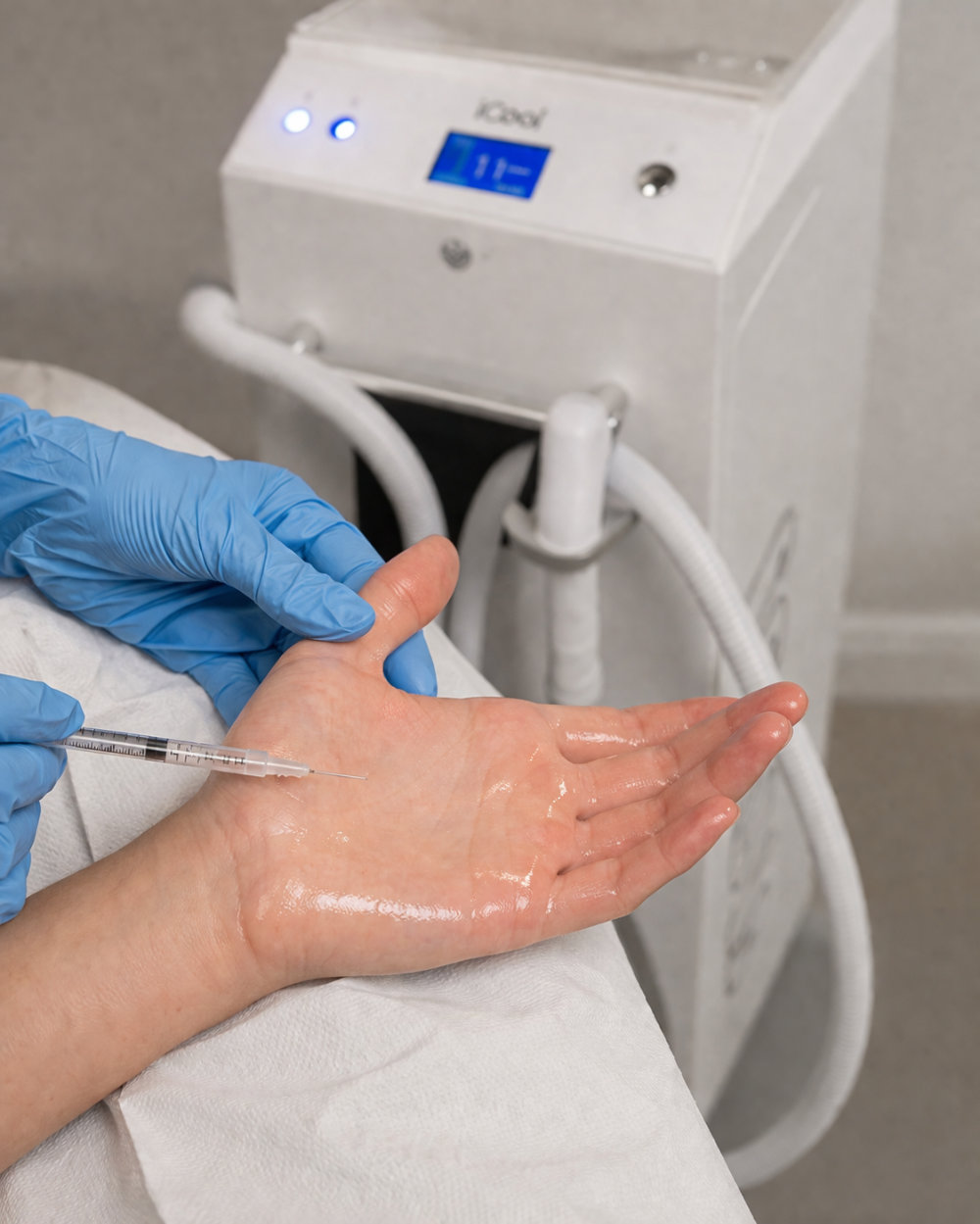
Treatment involves multiple small injections across the affected area.
Pain can be a concern, particularly for hands.
We now use a medical chiller device, which has made a significant difference:
- Continuous cooling during treatment
- Improved comfort, even in sensitive areas
- Allows us to focus on delivering effective results
Pain control is something we prioritise heavily.
How effective is it?
Botox for hyperhidrosis is one of the most consistently successful treatments we offer.
Patients typically notice a significant reduction in sweating within 1–2 weeks, with results lasting several months.
Menopause and sweating
A slightly different, but increasingly common, presentation is menopause-related sweating.
Patients will often ask whether excessive sweating can be a sign of menopause, and in many cases, it can.
Vasomotor symptoms (hot flushes and night sweats) are the most common feature of the menopausal transition.
These are driven by falling oestrogen levels, which affect the hypothalamus, the body’s temperature regulation centre, making it more sensitive to small changes.
This can lead to sudden flushing, heat, and sweating, often affecting:
- Scalp and hairline
- Forehead
- Underarms
- Chest and back
HRT is typically very effective for these symptoms.
However, not all patients want or are able to take hormones.
There are also non-hormonal medications available, and in some cases, targeted treatments such as Botox can be helpful for managing localised sweating, particularly on the face or scalp.
A few things people don’t realise
- It is not related to hygiene
- It is usually symmetrical
- It is often longstanding before patients seek treatment
- It can affect areas like the scalp, changing how hair behaves day to day
- Menopause-related sweating can feel just as impactful
In summary
Hyperhidrosis is not just sweating. It is something that can affect confidence, comfort and everyday interactions in subtle but persistent ways.
Underarm sweating remains the most commonly treated area, but hands, scalp and other regions can be just as impactful.
Botox offers a highly effective, targeted treatment, with results lasting around 4–6 months. Other options such as iontophoresis, MiraDry and newer technologies can also play a role.
And while it may become more noticeable in summer, for many people, it has been part of their daily life for much longer.
If this is something you have been dealing with, it is always worth a conversation.


